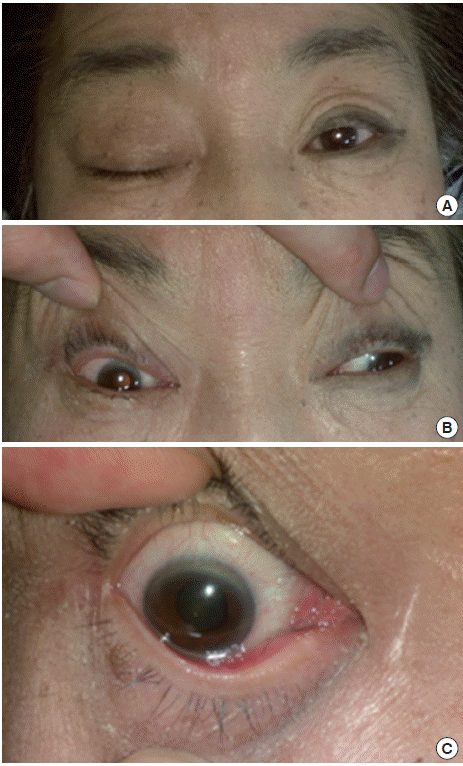
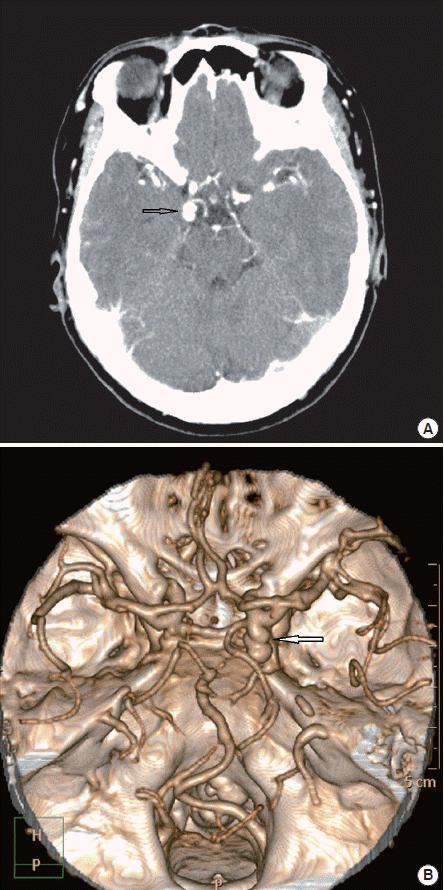
A 64-year-old woman with a history of diabetes mellitus and smoking was admitted to the emergency department because of headache, vomiting, binocular diplopia and right-sided ptosis. Five days earlier, she had a sudden headache of a stabbing nature in the right frontal area, which recurred every 5 hours. The visual analogue scale (VAS) score for pain was 8. Three days later, she noticed binocular diplopia and right-sided ptosis (Fig. 1A, B). Neurologic examination revealed right-sided third cranial nerve palsy with ipsilateral pupil dilation and no other definite focal neurologic deficits. Computed tomography (CT) scan and CT 3-D angiography revealed a 1-cm saccular aneurysm with lobulated contour in the right posterior communicating artery (Fig. 2A, B). On neurosurgical consultation, coil embolization of the aneurysm was performed successfully. The initial symptoms improved after 2 weeks and completely resolved after a 3-month follow-up in the outpatient department.
Unless proven otherwise, acute third cranial nerve palsy with ipsilateral pupillary dilatation is caused by a posterior communicating artery aneurysm [1]. Concomitant headache is a frequent symptom [1,2]. Expansion of such aneurysm may cause compression of the outer fibers of third cranial nerve palsy [1,2]. The pupillomotor fibers are located in the outer portion of this nerve; therefore, the pupil becomes dilated on the affected side. The posterior communicating artery can rupture spontaneously [3,4]. Treatment involves emergent blood pressure reduction if hypertensive, and neuroimaging and neurosurgical intervention [5].