INTRODUCTION
Patients with nontraumatic headaches have an important place in emergency room admissions [1]. There are primary headaches such as migraine, tension-type, cluster-type, as well as secondary headaches that occur due to a specific cause when examined [2]. The approach for nontraumatic headaches in the emergency department (ED) focuses mostly on recognizing those at risk of rapid deterioration, morbidity, and mortality among patients with headaches. Thus, it is important to quickly recognize high-risk headache situations in the ED and to offer appropriate treatment. Benign conditions constitute the majority of causes when the etiology of patients with nontraumatic headache is examined [3]. The first step in headache management is to identify high-risk situations. For headaches, it accounts for only 4% of high-risk headaches, but 10% to 14% of sudden onset headaches are thunderclap headaches [4,5]. Thunderclap headache requires urgent and detailed evaluation because it is associated with intracerebral aneurysm leakage (sentinel hemorrhage or suspected bleeding).
Antiplatelets and anticoagulants are commonly used in treating or in the prophylaxis of many diseases in recent years. Patients using these drugs have been known to have increased risk of intracranial injury after head trauma and worsening clinical outcomes [6]. Consequently, the risk of nontraumatic headaches due to intracranial hemorrhages (ICHs) caused by antiplatelet and anticoagulant therapy has also increased in recent years [7]. There is insufficient information on the indications in neurological imaging associated with the use of these drugs in patients admitted to the ED with nontraumatic headaches in the literature. Therefore, neurological imaging methods in the ED should reconsider excluding the underlying life-threatening conditions in patients presenting with nontraumatic headaches [8]. Noncontrast computed tomography (CT) is the most appropriate and fastest initial imaging examination in patients presenting to the ED with headache, and are the most sensitive in detecting acute ICH [9-11]. This study aims to investigate the association of antiplatelet or anticoagulant use on brain CT findings in patients admitted to the ED with nontraumatic headache.
METHODS
Study design and setting
This was a single-center prospective observational study. Patients admitted to the ED of a tertiary university hospital with nontraumatic headaches were included. Brain CT results with and without hemorrhage findings were compared. Ethics committee approval was obtained from the ethics committee of Akdeniz University School of Medicine (No. 30.11.2016/617). Written informed consent was obtained from the patients and/or their family members.
Selection of participants
Patients >18 years of age admitted to the ED with complaints of nontraumatic headache between May 1, 2016 and September 1, 2016 were included in the study. Patients ≤18 years of age and with a history of head trauma within the last 3 weeks were excluded. Headaches were classified according to the International Classification of Headache Disorders before brain CT was performed [2]. Ordering of an emergent brain CT was determined by the emergency physician based on the patient’s examination and international guidelines [9].
Data collection and processing
Triage staff and research assistants were trained on the study protocols and collected medical, clinical, and sociodemographic data of the patients in the standardized data form prior to CT. Anticoagulant and/or antiplatelet drug use by the patient was determined by the medical history and the Medula drug inquiry system. Patients with nontraumatic headaches were categorized according to brain CT indication after initial evaluation by the emergency physician. All brain CT images were reported by different radiologists with expertise in the field, and the results were recorded. Brain CT results were categorized into two groups, abnormal results (CT positive) and no abnormal results (CT negative), and compared. The CT positive group included patients who had any pathological signs on the brain CT and the negative group was considered as patients with a normal result (Table 1).
Statistical analysis
Data analysis was conducted using IBM SPSS Statistics ver. 20.0 (IBM Corp., Armonk, NY, USA). Categorical data were expressed as numbers and percentages and continuous variables were expressed as means and standard deviations. Chi-square test was used to compare categorical variables and the McNemar test was used for continuous data. A logistic regression analysis was performed to examine the association of independent variables with brain CT. A P-value less than 0.05 was considered significant.
RESULTS
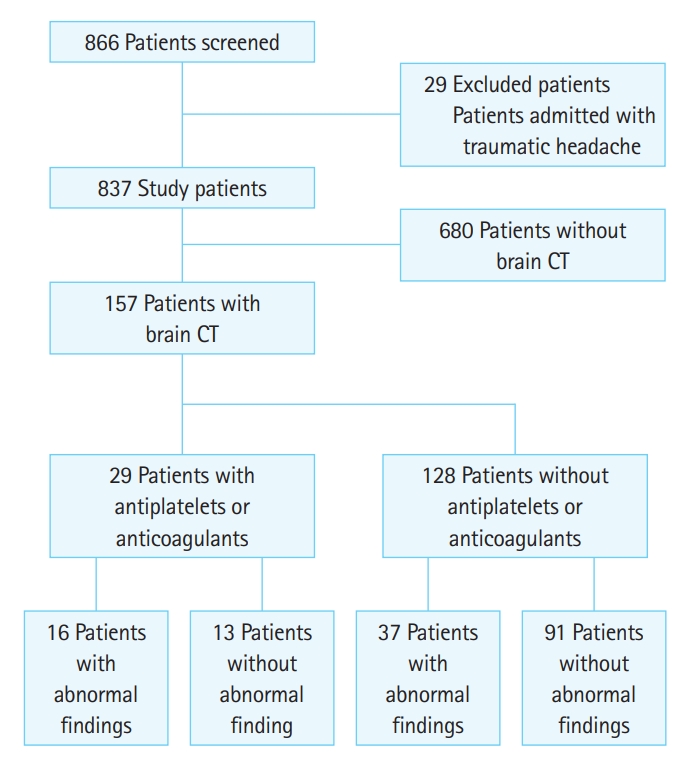
Between May 1, 2016 and September 1, 2016, 866 patients with headaches admitted to the ED were examined (Fig. 1) We included 837 patients in the study after 29 patients were excluded due to history of head trauma within the last three weeks. Of the patients included, 537 (63.4%) were female. The patient mean age was 40.2 years, and the median age was 38.0 years. Sixty-seven of these patients were using antiplatelets or anticoagulants. Of those 67 patients (8.0%), 28 were using aspirin, eight were using clopidogrel, two were using low molecular weight heparin, one was using unfractionated heparin, 11 were using warfarin, three were using a new generation of anticoagulants (two were using rivaroxaban, one was using apixaban), six were using aspirin+clopidogrel, three were using aspirin+warfarin, one was using low molecular weight heparin+warfarin, one was using aspirin+ticagrelor, and two were using aspirin+unfractionated heparin. Brain CT was requested for 128 of patients not using antiplatelets or anticoagulants and 29 of patients using these drugs. Of the 837 patients, 157 (18.8%) underwent brain CT scanning upon direction of an emergency physician (Fig. 1). Patients who had brain CT scanning were then analyzed. The mean age of these patients was 44.4±16.7 years. Among them, 88 patients (56.1%) were female. There were 39 patients (24.8%) with migraine headache, 45 (28.7%) with tension headache, 10 (6.4%) with cluster headache, 23 patients (14.8%) classified with other primary headaches, and 40 (25.5%) were classified as secondary headache (Table 1). Of the patients screened for brain CT with the decision of an emergency physician, 29 (18.4%) were using antiplatelets or anticoagulants. ICH was detected in two patients (0.01%) who were not using these drugs and three patients (0.10%) who were using these drugs. We discharged 134 patients (85.4%) and 23 (14.6%) were hospitalized after brain CT.
The association of antiplatelets or anticoagulants with CT results, hospitalization, and discharge was examined. Of the 29 patients using antiplatelets or anticoagulants, 16 (55.2%) were in the CT positive group. Of the 128 patients without antiplatelets or anticoagulants, 37 (28.9%) were CT positive. There was a statistically significant difference between both groups in terms of drug use (P<0.001) (Table 2). Regarding the patients’ disposition, 100 patients (96.2%) in the CT negative group and 34 (64.2%) in the CT positive group were discharged from the ED (P<0.001). Factors associated with CT results were examined in logistic regression analysis and a statistically significant association was found between the detection of positive results and antiplatelet or anticoagulant drug use (odds ratio, 2.478; 95% confidence interval, 1.003–6.102; P=0.048) (Table 3).
DISCUSSION
Antiplatelet and anticoagulant drugs are commonly used in diseases such as coronary artery disease, heart failure, atrial fibrillation, and stroke [12]. Previous studies have shown the efficacy of these drugs, and their side effects and risks have been discussed. The ICH rates were found to be similar in patients receiving aspirin or clopidogrel (0.2% vs. 0.4%) in the clopidogrel versus aspirin in patients at risk of ischaemic events (CAPRIE), African American Antiplatelet Stroke Prevention Study (AASPS), and management of atherothrombosis with clopidogrel in high-risk patients (MATCH) studies [13]. In addition, the incidence of ICH was 0.3% in patients using aspirin or aspirin+clopidogrel in the Clopidogrel for High Atherothrombotic Risk and Ischemic Stabilization, Management, and Avoidance (CHARISMA) study [14]. ICH was reported in 0.10% of patients admitted with headaches that underwent brain CT or used antiplatelets or anticoagulants in our study.
De Bonis et al. [15] investigated the association of antiplatelet/anticoagulant use with chronic subdural hematoma in the elderly patient population. Both anticoagulant and antiplatelet use were found to significantly increase the risk of chronic subdural hematoma. Furthermore, Gaist et al. [16] reported that antithrombotic use increased from 31.0 per 1,000 individuals from the general population in the year 2000 to 76.9 per 1,000 individuals in 2015. Out of 10,010 patients with subdural hematoma, 43.7% were shown to be using antithrombotic drugs. Low dose aspirin, clopidogrel, and oral anticoagulants were reported to have an increased risk of subdural hematoma in the same study. The use of antiplatelets/anticoagulants was not included as an indication of neuroimaging in nontraumatic headache patients admitted to the ED in the guidelines published by the American College of Radiology [17]. However, their use has been shown to be a risk factor for spontaneous ICH and chronic subdural hematoma in most studies [15,16].
There were not enough studies in the literature investigating the neuroimaging relationship in nontraumatic headaches using anticoagulant/antiplatelet drugs when we conducted this study. A recent study on neuroradiological results and etiology in nontraumatic headaches in the ED examined 1,132 nontraumatic headache patients and neuroimaging was performed in 303 patients and an intracranial anomaly was detected in 70 (23.1%) of the patients who underwent imaging [18]. Similarly, brain CT was not performed in more than half of our patient population in our study. However, it is noted that emergency physicians are more likely to perform brain CT (43.3% vs. 16.8%) if the patient has a history of antiplatelet/anticoagulant use. Out of 1,275 secondary nontraumatic headaches, 369 (28.9%) underwent CT scanning and 47 (12.7%) had intracranial pathological results within a 6-month period in another study on the application of computerized decision support systems for the indication of brain CT scanning for nontraumatic headaches in the ED [19]. The rate of CT positive rate among patients using antiplatelet/anticoagulant drugs was 16 (55.2%) in our study. The high rate of pathological results found in our study suggests a relationship between antiplatelet/anticoagulant drug use and CT scanning in nontraumatic headaches in the ED.
The present study has limitations. First, this was a single-center study. Second, brain CT could not be performed on all nontraumatic headache patients included in the study. This limitation suggests that there may have been abnormal intracranial results in patients without CT scan. All brain CT images were reported by different radiologists, so this may have affected the results. Additionally, brain CT decision-making was not always determined by the same physician. Multicenter prospective studies are required with larger patient groups with nontraumatic headaches using anticoagulants or antiplatelets in the ED.
The use of antiplatelets or anticoagulants in patients admitted to the ED with nontraumatic headaches are associated with increased risk of abnormal intracranial results on brain CT. It will be beneficial to include this group of drugs in neuroimaging indications in nontraumatic headache patients.