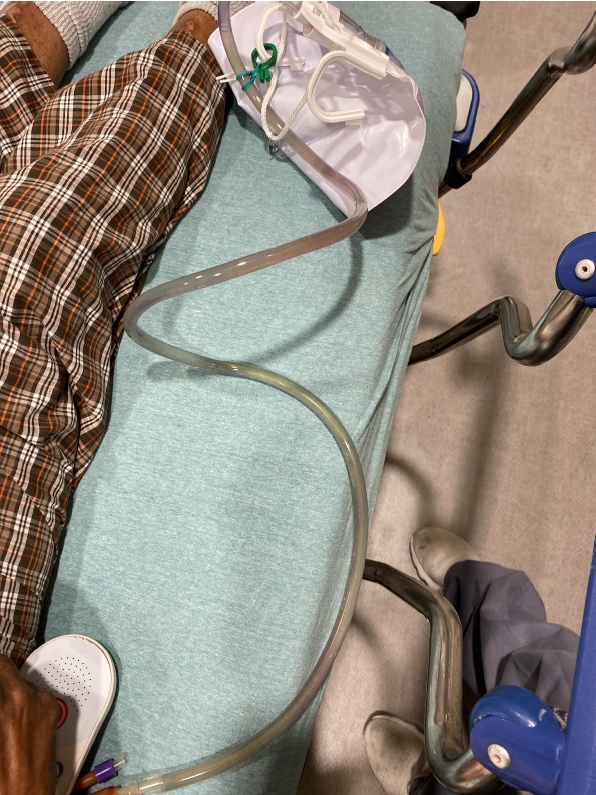
A 56-year-old male patient with a history of prior stroke and recurrent urinary tract infections (UTIs) with suprapubic Foley catheter presented to the emergency department with discolored urine. Physical examination demonstrated intact Foley catheter with the bag containing bright purple urine and yellow urine within the tubing (Figs. 1, 2). Urinalysis was positive for 1+ leukocyte esterase and 26 to 50 white blood cells and numerous bacteria. Urine culture was positive for Proteus mirabilis and Klebsiella pneumoniae. He was treated with third-generation cephalosporin for presumed UTI. The Foley catheter was not exchanged at this time but presented 2 days later and was noted to be without purple urine.
Purple urine bag syndrome (PUBS) is a discoloration of urine generally seen in patients with UTI. Predisposing patient factors include advanced age, long-term urinary catheterization, chronic kidney disease, increased dietary intake of tryptophan, alkaline urine, concurrent constipation, and ileus [1,2]. Bacteria that are implicated in its development include Escherichia coli, Proteus mirabilis, Klebsiella pneumoniae, and Pseudomonas aeruginosa [3]. PUBS is a benign condition that can occur when these gram-negative bacteria in urine convert tryptophan derivatives into pigmented metabolites. The derivative, indoxyl sulfate, is secreted into the urine where the sulfatases and phosphatases convert it into its two metabolites: indigo (a blue pigment) and indirubin (a red pigment) [2]. As these pigments interact with tubing of the Foley bag, a characteristically rare purple hue is produced. While isolated PUBS can be a benign finding, it may be associated with increased patient mortality and should alert the provider to investigate for underlying infection [3].