Dear Editor,
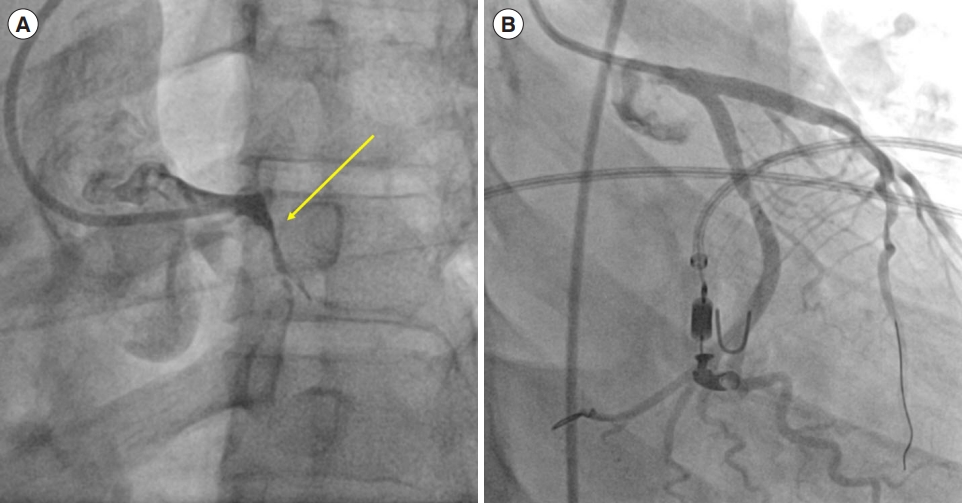
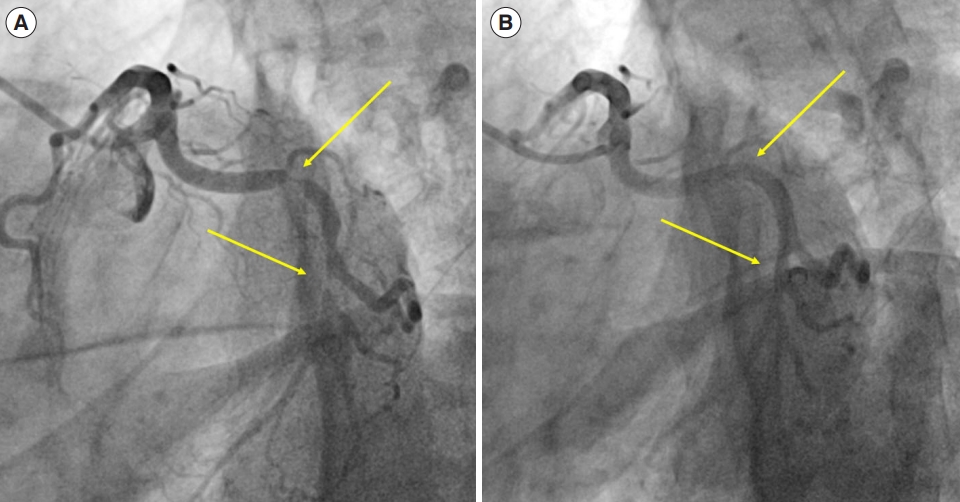
We present a case of deep clinical and educational interest, underlying the importance of a multidisciplinary approach in the diagnostic approach to chest pain. A 36-year-old Indian male patient presented to the emergency department complaining about episodes of oppressive chest pain over the past week. Physical examination showed normal chest and cardiac auscultation. An electrocardiogram (ECG) showed sinus bradycardia with no repolarization abnormalities. Cardiac troponin was elevated (high-sensitive troponin I [hs-TnI], 171 ng/L). The patient was affected by asthma, treated with beclomethasone/formoterol 100/6 μg one inhalation twice daily. He also reported allergic rhinitis, a previous allergic reaction to ketoprofen (cutaneous rash) and Raynaud syndrome. The patient conditions rapidly deteriorated due to acute cardiogenic shock and ECG modification with anterolateral ST-segment elevation. An urgent invasive coronary angiogram (ICA) was performed, showing a complete thrombotic left main occlusion, which was treated with angioplasty and two drug-eluting stents (Fig. 1). Echocardiography showed severe left ventricular dysfunction. A mild dermatitis after salicylic acid administration resolved with intravenous hydrocortisone bolus (1 g). Over the next few days, the clinical condition rapidly improved with recovery of normal ventricular function. The thrombophilia screening was negative. He was discharged on dual antiplatelet therapy (aspirin 100 mg and prasugrel 10 mg daily), as well as atorvastatin 40 mg and bisoprolol 1.25 mg daily. Two weeks later he returned to the emergency department with recurrent jaw and chest pain, responsive to sublingual nitrates. Cardiac troponin were elevated (hs-TnI, 106 ng/L), with no clear ECG abnormalities. An ICA was performed, showing a good angiographic result of the recent angioplasty and no other coronary stenosis. During the hospital stay, the patient experienced several anginal episodes, responsive to nitrates. Serial ECGs during chest pain showed ischemic alterations in different leads, suggesting different coronary territory involvement, with troponin level fluctuations. During a longer angina episode, an ICA was repeated, and coronary vasospasm of the circumflex artery were detected, with complete resolution after intracoronary nitroglycerin (Fig. 2). A diagnosis of vasospastic angina was made, and nitroglycerin and calcium channel blockers were added. However, several vasospastic anginal episodes still occurred on a daily basis. Cetirizine was added to the therapy, suspecting coronary ischemia secondary to allergic reaction (Kounis syndrome), without any effect on symptoms. Further investigations were made: laboratory tests revealed eosinophilia (4,390 cells/μL), increased C reactive protein (9.4 mg/L) and positive antinuclear antibodies (1:320).
Other serological and immunological tests were negative, including proteinase 3 and myeloperoxidase antineutrophil cytoplasm antibodies (ANCA). An abdomen and chest computed tomography scan were performed and both were negative. Eosinophilia and a history of asthma led to suspected eosinophilic granulomatosis with polyangiitis (EGPA). The patient was treated with intravenous methylprednisolone 250 mg once daily for 3 days, followed by oral prednisone 1 mg/kg daily, with rapid and complete disappearance of the recurrent angina episodes. Intravenous cyclophosphamide was started, after sperm cryopreservation and continued for 6 months. A maintenance therapy with azathioprine was started
The presented case demonstrates how coronary involvement in EGPA can mimic coronary artery disease. Only an accurate evaluation of biomarkers and patient medical history correctly pointed the diagnosis towards an isolated coronary vasculitis causing myocardial infarction (MI) as an atypical manifestation of EGPA, prompting early immunosuppressive therapy pivotal for the patient survival. The patient did not fulfill the 1990 American College of Rheumatology (ACR) classification criteria for EGPA. Nevertheless, the presence of late-onset asthma and allergic rhinitis, eosinophilia greater than 10% on white cell differential count and the excellent clinical response after administration of high-dose corticosteroids confirmed the diagnosis of EGPA [1]. Asthma is the key clinical feature and is found in more than 90% of EGPA patients [2]. It usually presents about 8 to 10 years before the vasculitic phase [3]. Cardiac involvement is common and represents one of the most serious manifestations of EGPA. It accounts for approximately one-half of deaths attributable to EGPA. Cardiac clinical manifestations include cardiomyopathy with signs of heart failure, pericarditis, cardiac rhythm abnormalities and—less frequently—coronary vasculitis [4]. Even if cardiac involvement in EGPA is well reported in the literature, isolated coronary vasculitis causing acute MI is a rare manifestation, especially at disease onset. Coronary vasculitis associated with EGPA may present with vasospasm, coronary thrombosis, and coronary ectasia [5]. To our knowledge, this is the first case reported in the literature where coronary vasculitis resulted in both thrombosis and vasospasm. At the time of first hospital admission, a left main complete thrombotic occlusion with associated vasospastic features was detected, and coronary vasospasm was also documented in the following admission. Interestingly, the patient did not experience recurrent angina during the first hospital stay. We believe this was due to the fact he received intravenous corticosteroids to treat a mild dermatitis after aspirin administration, temporarily improving coronary inflammation. Corticosteroids and immunosuppressive treatment are the mainstay of induction therapy in severe forms of EGPA and usually result in the recovery of impaired cardiac function. At 8-month follow-up, the patient was completely asymptomatic with normal biventricular function.